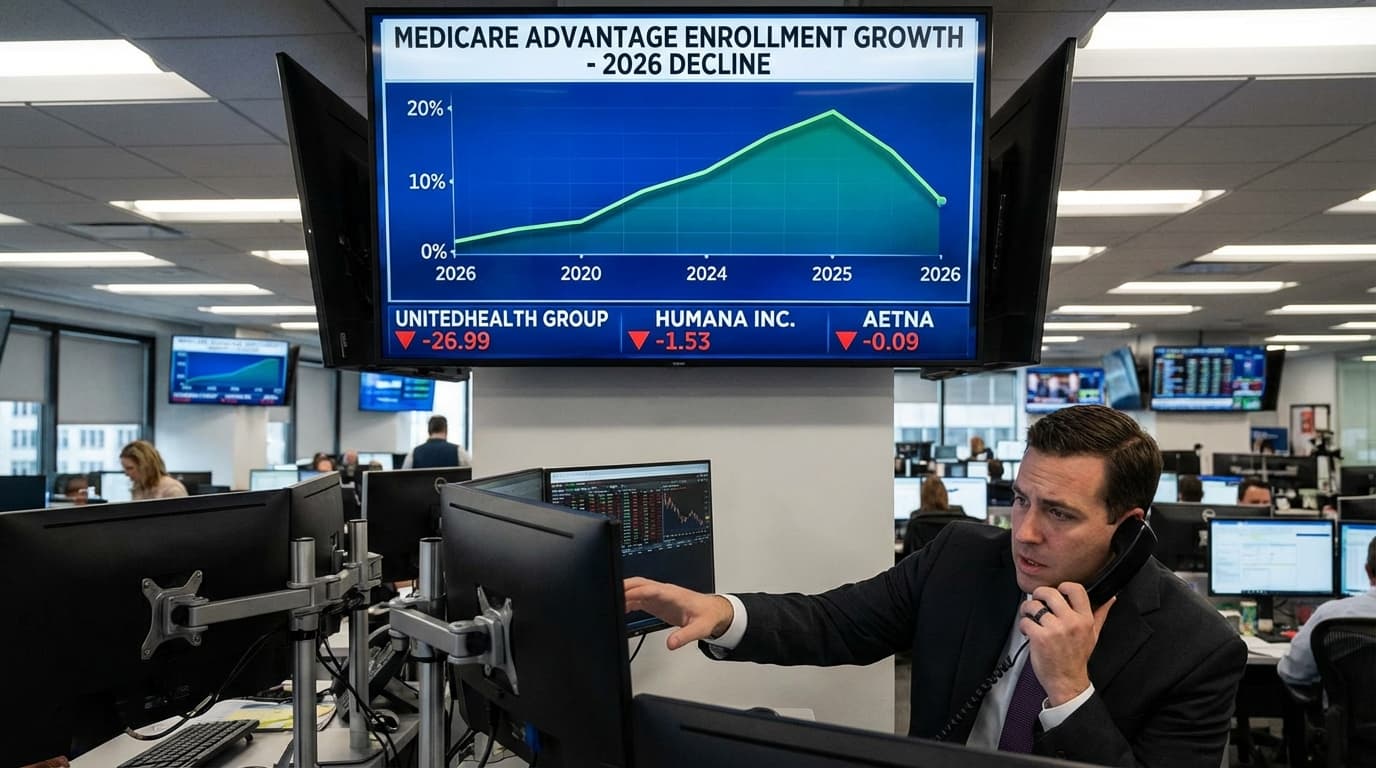
Medicare Advantage Growth Declines for Second Consecutive Year Amid Industry Changes
Medicare Advantage, a key segment in the healthcare insurance landscape, has experienced dwindling membership growth as several leading insurers, including UnitedHealth, Humana, and Aetna, have been actively reducing their rolls. This development follows a series of changes affecting the program and could signal a major shift in the sector.
Medicare Advantage, a critical insurance option for millions of Americans, has seen its membership growth rates diminish for the second consecutive year in 2026. This deceleration emerges amid significant structural changes and strategic moves by prominent insurers such as UnitedHealth, Humana, and Aetna, which have reportedly been working to decrease their Medicare Advantage membership rolls.
Medicare Advantage, also known as Medicare Part C, offers beneficiaries an alternative to original Medicare by providing coverage through private health plans that often include additional benefits. Over recent years, this program experienced robust growth, becoming a dominant force in the Medicare landscape. However, recent data indicates a slowdown in enrollment expansion, which might be attributed to various industry and policy adjustments.
The reported efforts by major insurers to reduce their Medicare Advantage membership could be strategic responses to evolving financial and regulatory environments. Factors such as changes to payment models, increased scrutiny on plan benefits, and rising operational costs may contribute to their cautious approach toward growth.
Furthermore, the market dynamics within Medicare Advantage are influenced by competitive pressures and shifting beneficiary preferences. Insurers may be recalibrating their strategies to focus on quality of care and cost management rather than aggressive membership acquisition. This realignment may affect plan offerings, provider networks, and ultimately, patient experiences.
The implications of this trend are multifaceted. For beneficiaries, reduced growth might translate to fewer plan choices or modified benefits. For the healthcare system, a slowing Medicare Advantage expansion could impact federal expenditures and the broader insurance market.
Looking ahead, stakeholders including policymakers, insurers, and healthcare providers must closely monitor these developments. Understanding the drivers behind membership adjustments and navigating the complex healthcare policy landscape will be essential to ensuring that Medicare Advantage continues to meet the needs of older adults and other eligible populations.
This trend also highlights the importance of adaptive strategies in the insurance sector amid a changing healthcare environment that balances regulatory compliance, financial sustainability, and patient-centered care.
For a comprehensive analysis and further details, see the original report at STAT News: https://www.statnews.com/2026/02/16/medicare-advantage-membership-growth-2026-unitedhealth-humana-aetna/?utm_campaign=rss
Join the BioIntel newsletter
Get curated biotech intelligence across AI, industry, innovation, investment, medtech, and policy—delivered to your inbox.